August 1, 2023
In my article, “Reducing Intraocular Pressure is an Added Benefit of Cataract Extraction,” I wrote about the joy I feel when diagnosing a patient with a cataract. That joy is because of the wonderful opportunity we have to vastly improve, not only the vision, but also the lifestyle of the patient. For the primary care optometrist there is another avenue for professional enjoyment around the cataract process. Rather than just “co-managing” the post-operative course of cataract surgery, the referring doctor should “manage” every step of the cataract process. Here are the hows, but more important, the whys behind this statement.
The Traditional Process
In most instances, the optometrist makes the diagnosis of a cataract, gives a brief explanation of what a cataract is, a briefer explanation of what the surgical process entails, and finally a quick mention that she will be referring the patient to “The Surgeon” for this procedure. At this point, usually, the OD or her tech will inform the patient that the surgeon’s office will contact the patient directly for the consultation, and the patient is checked out with no follow-up appointment made for the optometrist.
At the heart of this process is a hope and a prayer that the surgeon’s office will actually call the patient, understand what the appointment is for, return the patient to the optometrist for post-operative management, and bill properly using the appropriate codes for co-management. What could possibly go wrong? If you have ever spent time in a busy cataract surgeon’s office, you already know the answer to that question. There are plenty of opportunities for a communication screwup to occur.
When your patient gets to the surgical office, he or she will be met by an onslaught of personnel, paperwork, and likely impersonal treatment, especially when compared to what they are used to in your office. The patient will have multiple encounters with multiple staff members, and in all likelihood, will see the surgeon for about five minutes. Hopefully, the surgeon will agree with your diagnosis and treatment recommendation.
At that point, the fun really begins. The patient then is ushered to a surgical coordinator who will discuss the different intraocular lens (IOL) options and spend a great deal of time adding to the confusion. After this two-hour experience, your patient, who is used to the caring staff in the optometrist’s office, is often left bewildered and wondering why their cataract surgery will not be covered by insurance.
The Enlightened Process
I believe the optometrist’s role in this process should not end at the referral. As a matter of fact, I feel that it is an abdication of your duty as the primary eye care provider if this occurs. I believe that, when the optometrist has made the diagnosis of cataracts, the role as the “manager” of the process just begins. The OD should discuss with the patient the details of cataract surgery, how it is performed, and in which facility the surgery will take place (hospital setting or ambulatory surgical center, for example). Also, the post -operative course should be discussed as well as the responsibility of using any drops post-operatively. It is also incumbent upon the managing optometrist to have a discussion with the patient around the different types of IOLs available and offer a recommendation as to which type is needed. This is extremely important as the surgeon will not know your patient’s eyes as well as you do, and the staff at the surgeon’s office certainly doesn’t understand the needs of your patient like you do. Discussing options and ultimately recommending a certain type of IOL for your patient is, in most cases, the most important part of this journey.
Selecting the Best IOL
Before the optometrist can have this discussion, though, she needs to be aware of the different types of IOLs and specifically, which type of multifocal IOLs that the surgeon with whom she co-manages is currently using. A discussion with the surgeon about which IOLs are being chosen and the nuances as to why the surgeon chooses one IOL over another are both important to understand. By knowing indications for certain IOLs, the referring OD can better recommend suitable options for the patient. Here are a few examples:
First, an easy one, if your patient has been a successful monovision contact lens wearer and develops cataracts, the best solution is likely to use monofocal IOLs to mimic the monovision type of vision that this patient has become accustomed to. It is much more successful for the patient to continue in monovision rather than to use prescription readers or try to adapt to the visual situation created by multifocal IOLs. But if a surgeon has not been aware that this particular patient has been successful in monovision, it is highly unlikely that this option will be even presented to the patient. If the managing doctor believes that monovision is the best option, then that should be strongly conveyed to the surgeon.
A second example is one in which the patient exclaims, “This is great! I won’t have to wear glasses ever again!” They have heard that somewhere, and it may actually be stated at the surgeon’s office. But the likelihood of a pseudophake never needing glasses ever is very rare. Even in an exceptionally performed cataract procedure where multifocal IOLs were implanted in both eyes, your patient will likely need a prescribed set of eyeglasses sometimes. Whether it is prescription readers, anti-reflective lenses for computer usage, or spectacles for driving at night, some form of eyewear will almost always be indicated. Failure to discuss this with your patient will ultimately lead to a dissatisfied pseudophake, who will likely blame the optometrist for visual woes. Taking five or 10 minutes pre-operatively to discuss options and listen to your patient’s hopes for a post-operative outcome, will greatly increase the satisfaction with the procedure for both parties.
Finally, once you have completed this discussion, once you have elicited what type of IOLs will be best for your patient, the managing OD needs to do two more things. First, have the discussion about how much these options will cost out of pocket. Any IOL other than a monofocal has an upcharge that Medicare or other insurances will not cover. I believe that the referring doctor should understand what these non-covered services cost and be able to have that discussion with the patient. If you feel that your patient would benefit from a specialty IOL, then you should present the fee structure as well. The best surprise is no surprise at all, especially when it comes to money.
The last step of the proper referral is to compose a pre-operative referral to the chosen surgeon. This note should outline not only the diagnosis and proposed procedure, but it should also denote your recommendation for your patient. If you and the patient feel a standard monofocal IOL is best, make that clear. Likewise, if a multifocal IOL system is warranted and recommended, make that choice clear. Be an advocate for your patient and be the doctor who makes the proper recommendation. Doing so will result in a much more rewarding process for everyone.
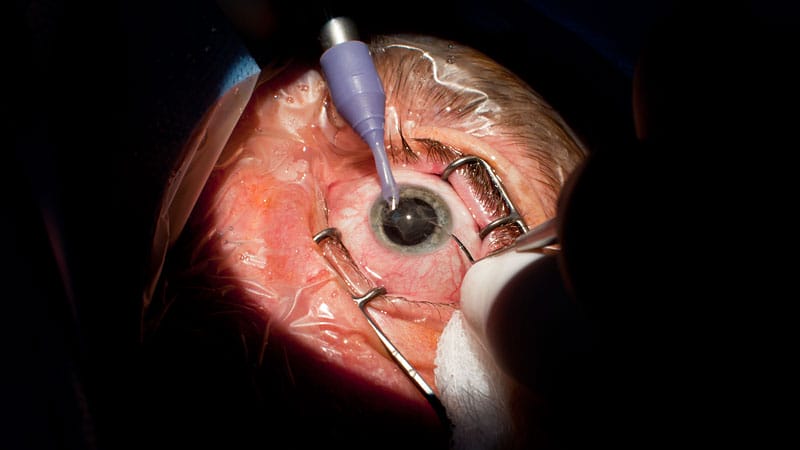
Photo: Dreamstime